Blood sugar testing is a relatively simple process that can reveal a wealth of valuable information about your health. From early detection of diabetes (and pre-diabetes) to healthy weight loss and stable energy levels, we recommend that all Heads Up Health users complete some basic testing to understand their blood sugar.
Yes, you will need to prick your finger to draw a droplet of blood. Yes, it sucks at first. But stick with us (pun intended) for the remainder of this post. Hopefully we can convince you that the benefits of testing and educating yourself on blood sugar far outweigh the modest discomfort.
Heads Up Health was designed to help you track your blood sugar along with all of your other important health data. You can get started now using the button below. Or, read on for for some great reasons to consider your own blood sugar testing along with some information to get your started.
[maxbutton id=”1″]
Benefits of blood sugar testing – establish your own baseline
Our own unique blood sugar responses are a function of our genetics and our own unique lifestyle choices up to this moment in time. One person’s body may tolerate a burger and fries just fine, while the other may see their blood sugar levels go through the roof from the very same meal. Do you know how well your body’s blood sugar mechanisms would handle a burger and fries? What about your favorite breakfast? You should know these numbers. They have important implications for your long-term health and wellness.
The only way to know your own body’s tolerance is to perform your own blood sugar testing and gather your own data. The data can help you learn which choices make the most sense for your own body.
Benefits of blood sugar testing – assess your risk for diabetes (or pre-diabetes)
You may be thinking “I am not diabetic – why should I check my blood sugar?” Great question. The reality is that one in three Americans will develop diabetes or pre-diabetes in their lifetime. Pre-diabetes is defined as having a fasting blood sugar of between 100-125 mg/dL. What’s your fasting blood sugar? How close are you to pre-diabetes? Everyone should know this answer and yet few people do.
Assessing your risk now with some simple testing could help you make healthy changes years before any serious symptoms develop.
Benefits of blood sugar testing – stay lean n’ mean
One of the best ways to keep the fat off over the long run is to consume foods that keep blood sugar low. This means reducing calories from sugar, refined carbs and processed foods with calories from healthy fats, protein, vegetables and low-sugar fruits.
Blood sugar testing can help you choose foods that support weight loss
The key to healthy weight loss is to eat meals that keep you full and satiated without sending your blood sugar through the roof! Testing your blood sugar before and after you eat different meals can help you learn which foods are most favorable when it comes to optimizing your own blood sugar response.
Benefits of blood sugar testing – reduce or eliminate medications
Metabolic diseases such as Type II diabetes and obesity can be treated and even reversed with the right lifestyle changes (e.g. ketogenic, paleo and other ancestral-based diet and lifestyle interventions), thereby reducing or eliminating the need for prescription medications. Learning how to master your blood sugar through regular testing can be an important tool in this process.
In many cases, once blood sugar stabilizes through proper diet and lifestyle modification, many other symptoms improve as well including hypertension, high cholesterol, poor sleep and weight gain, which can further reduce the need for medications.
Benefits of blood sugar testing – Outsmart the food companies
We really wish we could say that all the food companies out there have our best interests at heart – but sadly that’s just not true. Sugars and refined carbohydrates are in everything we eat these days and the effects on our blood sugar (and ultimately our health) can be disastrous. Additionally, refined and processed carbohydrate-based foods are cheap to produce and highly profitable for food companies.

Testing before and after meals is an excellent way to learn which foods are harmful vs. helpful for your blood sugar
What’s more, food companies are constantly coming up with clever new names for sugar and high-fructose corn syrup-based products to sneak them past our label-reading defenses. However, there’s one defense the food companies can’t get past – and that’s some real blood sugar data collected from your own body. Testing your blood sugar after you eat is a foolproof method of figuring out which foods to eat and which to avoid for stable blood sugar.
Getting Started
Here are a few simple steps to get you started on the path of blood sugar testing:
Step 1 – Purchase a glucometer
You can find affordable models at your local pharmacy or online. I personally use the Keto-Mojo dual-purpose glucose and ketone meter and have found it to be accurate and reliable.
Step 2 – Test yourself
Here are some of the best times to test your blood sugar along with some information on how to assess your results:
In the morning (fasting glucose):
Fasting glucose is taken after a period of not eating for at least eight hours. Typically first thing in the morning before breakfast is the ideal time to take this reading. Compare your fasting readings to the table below.
Table 1: Reference ranges for fasting blood sugar
| Hypoglycemia (low blood sugar) | <70 mg/dL |
| Normal | 70-99 mg/dL |
| Pre-diabetes | 100-125 mg/dL |
| Diabetes | Two consecutive fasting readings at or above 126 mg/dL |
What to look for: Notice how different lifestyle choices affect your fasting blood sugar. For example, regular exercise and switching to a low-carb/high-fat diet are great experiments you can conduct on your own to lower your fasting glucose.
Regularly testing different lifestyle changes and conducting your own n=1 experiments will help you develop the ability to exert control over your blood sugar, which can be very empowering. Work with a health professional who can help you get started and to learn how to interpret the numbers. We recommend checking out PrimalDocs.com for a list of health experts in functional and ancestral medicine.
Before meals (pre-prandial) & after meals (post-prandial)
Check your blood sugar before meals to get your baseline reading. Check again one hour and two hours after your meal and compare your results to the table below. Take note of which foods drive blood sugar highest. Typically these are meals that are high in sugar/fructose and processed carbohydrates (bread, pasta, cereal etc.). Conversely, foods that keep you feeling full and support stable blood sugar are centered more around vegetables, healthy proteins and healthy fats.
The table below is from the American Diabetes Association and provides some guidelines on post-prandial (after eating) blood sugar:
| 2-hour post-prandial | |
| Normal | <140 mg/dL |
| Pre-diabetes | 140-200 mg/dL |
| Diabetes | >200 mg/dL |
While the table above aims for a target of below 140 mg/dL, it is possible to keep this even lower. Try choosing meals that keep blood sugar below 120 mg/dL at the one-hour and two-hour post-prandial mark. You may also want to take a reading three hours after your meal. By this time, levels should be close to what they were before you ate.
Step 3 – Make the adjustments
As you learn the connection between diet and lifestyle and their effects on blood sugar, you can begin to make changes necessary to support your health goals.
Strategies for lowering blood sugar include the following:
- Dietary change: Adopting a low-carb/high-fat diet (and lifestyle) based on paleo, ketogenic or ancestral principles is one of the most effective ways to support stable and healthy blood sugar.
- Get more exercise: Exercise and lean muscle mass essentially “mop up” excess glucose circulating in our system and can help lower blood sugar.
- Improve sleep quality: Getting high quality sleep can also help lower blood sugar. Consider a diagnostic sleep study if you suspect you may have sleep apnea and work on adopting good sleep hygiene techniques.
- Lower stress levels: Lowering stress through meditation, exercise and healthy social interactions can also help support stable blood sugar.
Step 4 – Track your progress
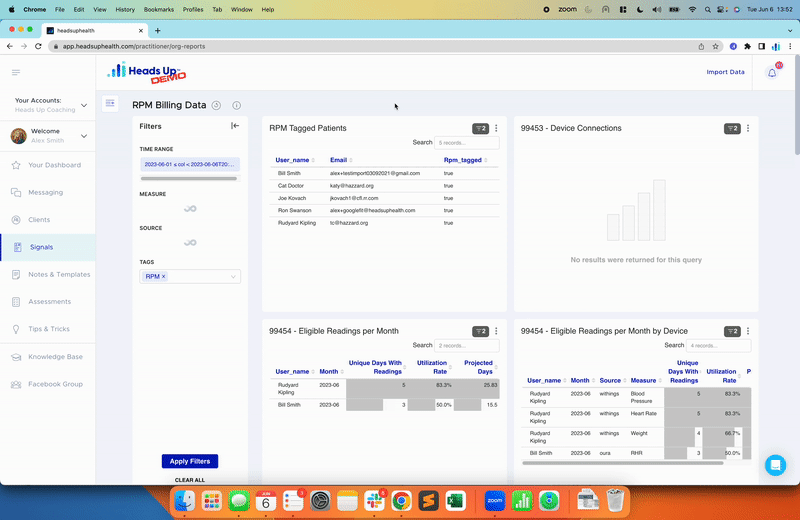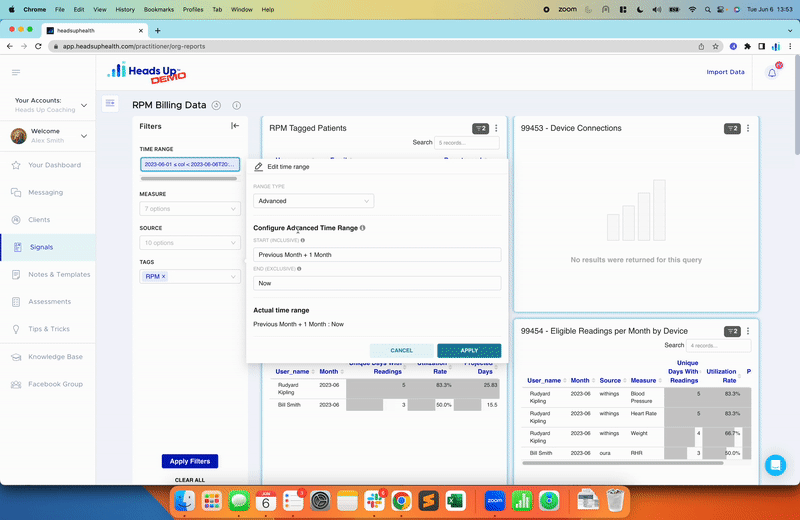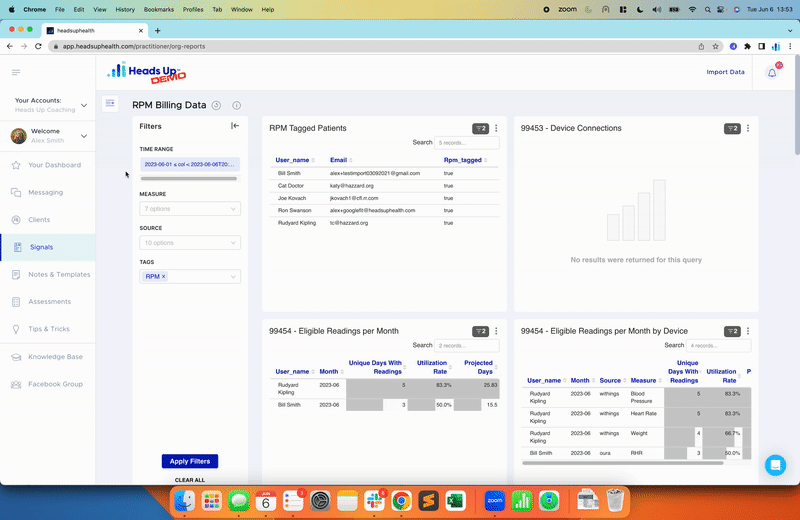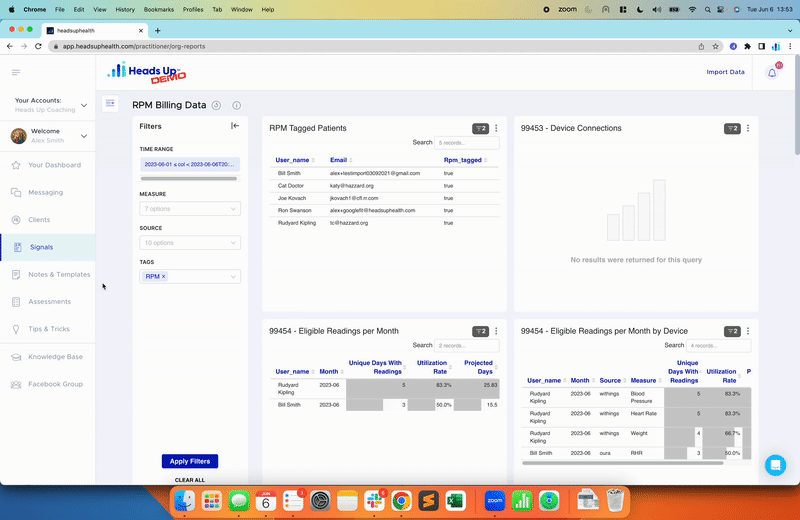
Heads Up Health was designed to help you track all of your health metrics in one place. From blood sugar to body fat percentage to cholesterol readings. We’ve built some advanced features into our software specifically for blood sugar tracking.
For more videos on health tracking with Heads Up Health, check out our YouTube channel.
Summary
Learning how to track your body’s blood glucose level is an essential tool for long-term health, weight management, disease prevention and much more. There are many factors at play when it comes to blood sugar levels and everyone’s body responds differently. Hopefully the points above provide some introductory guidance on how you can employ blood sugar testing for your own health efforts. Getting started is easy and we’ve outlined some simple steps that can get you started. Speak to your doctor if you have questions or contact us, we are here to help.
[maxbutton id=”1″]











Thanks, team Ambrosia for creating Nightrider BluCon that has made my life much simpler. Now, I don’t have to worry when my glucose level will rise or fall, as I will get an alert. I will recommend your life-changing products to all people with diabetes and want to have a better way to tackle it.